Maximus, a healthy 6-month-old mixed breed neutered male cat, was presented for severe thermal burns over large areas of his body after jumping into a bathtub filled with scalding hot water. The injury occurred just a few hours before presentation.
On admission, Maximus was tachycardic and severely painful. All four paws were red, swollen, and bleeding. The skin on his ventral abdomen and thorax was bright red and bruised. It appeared that the injury affected about 50% of his body. There was no other previous history of medical problems.
Initial Treatment
Maximus was initially administered intravenous fluids, antibiotics, and buprenorphine for pain. Continuous intravenous infusion of fentanyl was added to the treatment regimen soon after admission. Blood tests showed evidence of dehydration and elevated serum potassium. Silver sulfadiazine was used as the topical cream medication on the burned areas.
Maximus was non-ambulatory because the skin of his footpads was peeling off, leaving subcutaneous tissue exposed. Over the next several hours, the burned areas on his legs, chest, and belly gradually became purple in color. Some of the burned skin on his chest was becoming hard and leathery. (Fig. 1a,b) On a pain scale from 1-24 (1 being little or no pain, 24 being the worst pain possible), the attending clinician listed Maximus as 24. Intravenous lidocaine and ketamine were added to the fentanyl infusion to provide more analgesia. The dosage of fentanyl was also increased.
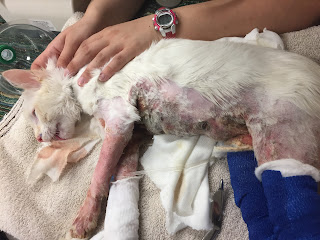 |
| Fig. 1a: Maximus several hours after admission to the hospital |
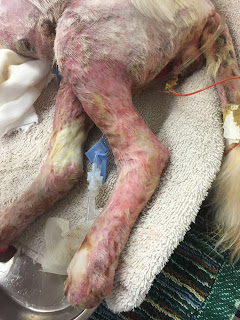 |
| Fig. 1b |
After sedating him with intravenous propofol, all of Maximus’ burned areas were carefully clipped and cleaned. With the hair removed, the burned regions were more clearly visible; the total surface area of his burned body appeared to be closer to 60%.
More blood tests showed that Maximus’ albumin was already below normal. Albumin was being depleted because of the severe inflammation of the damaged skin and loss of albumin-rich fluid that oozed from his wounds. A nasogastric tube was placed to augment his dietary intake.
Wound Management
On day two after admission, Manuka honey (Medihoney) was begun as the topical medication on the wounds, and standard bandaging was continued. The burned areas were gradually declaring themselves, and on day 4, some were starting to turn yellowish-brown and becoming hard and crusty. Escars were developing, indicating full-thickness skin injury. (Fig. 2)
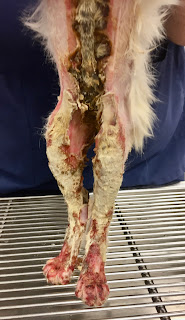 |
| Fig. 2: Escar development over mid abdomen and rear legs |
To simplify the bandage changes that were time-consuming and painful, the attending clinician Dr. Becky Ball began covering Maximus with infant onesies, little pajama outfits that completely covered the entire body, legs, and feet. (Fig. 3) Each day the onesie was removed, the wounds gently cleaned, Medihoney ointment applied, and a clean onesie replaced.
 |
| Fig. 3: Onesie pajama bandage applied. |
Maximus was discharged 12 days after admission. The owner, a physician, assumed the nursing care at home. Rechecks with Dr. Ball were scheduled every 4-5 days for wound assessment. The escars gradually peeled away from the healthy skin, exposing new granulation tissue underneath. No evidence of infection was seen, and Maximus' appetite was good.
Maximus continued to be re-examined about every two weeks. The eschars completely sloughed off, and the skin defects were contracting and closing well. But, as the skin tightened in his inguinal region, scar tissue pulled his rear legs medially, severely restricting his mobility. (Fig. 4) Surgery would be necessary to alleviate the contracture and allow Maximus to use the hind legs better.
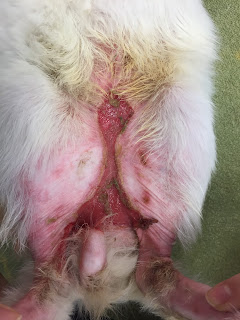 |
| Fig. 4: Wound contraction of inguinal skin. |
Skin Reconstruction
Seven months after Maximus’ injury, a caudal superficial epigastric axial pattern skin flap was performed to alleviate the inguinal wound contracture. (Fig. 5a-b) Click here for a detailed description of the skin flap procedure. The surgery went well, and he was discharged from the hospital the following day.
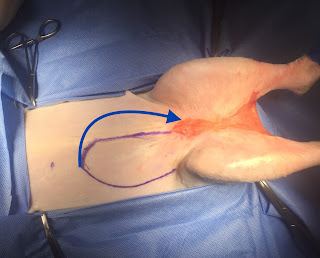 |
| Fig. 5a: Axial pattern skin flap design. Arrow indicates the direction of rotation of the flap after it is dissected out. |
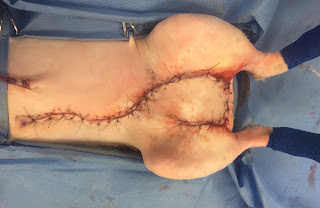 |
| Fig. 5b: Completed skin flap procedure. |
Seven days postoperatively, suture removal was performed. The skin flap was viable and had healed well to adjacent skin. Maximus was much more mobile and less painful. Seven months postoperatively, he was examined again and was doing well with all wounds healed and his function back to normal. (Fig. 6, 7)
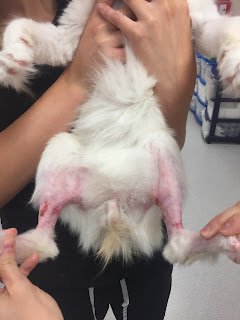 |
| Fig. 6: Appearance of inguinal area seven months after skin flap reconstruction. |
 |
| Fig. 7: Maximus and his owner 15 months after his injury. |
Discussion
Maximus overcame a severe injury with burns over a large portion of his body. He exemplifies the remarkable wound healing process, particularly when supported with good nursing care. Manuka honey was effective in preventing infection and encouraging wound healing. Dietary support was instrumental in avoiding hypoproteinemia and malnutrition. Excessive wound contracture necessitated skin flap reconstruction, improving mobility and relieving chronic pain.
Maximus' owner, a neonatologist, was instrumental in his recovery. She assumed the challenging nursing care at home and was diligent in the tedious work of medicating, bandaging, and maintaining good hygiene.
Maximus’ complete story is told in Dr. Birchard’s book: Their Tails Kept Wagging: Pets Show Us How Hope, Forgiveness, and Love Prevail, a collection of inspirational stories of severely ill pets who survived due to modern medicine and compassionate caregivers. For more information, click here.



No comments:
Post a Comment